A Rising Star


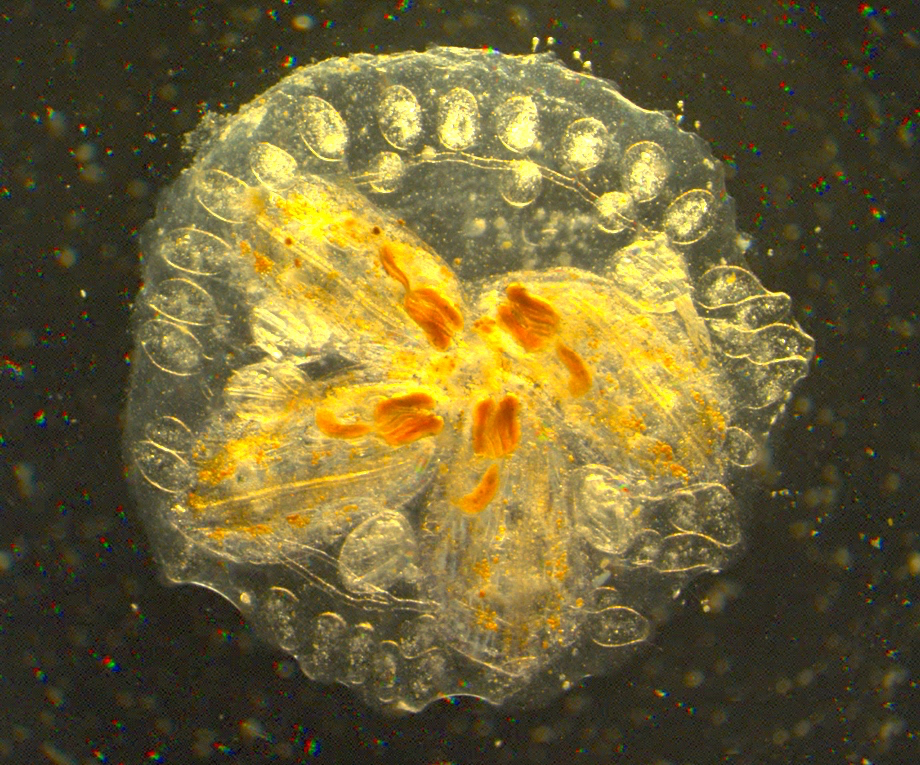
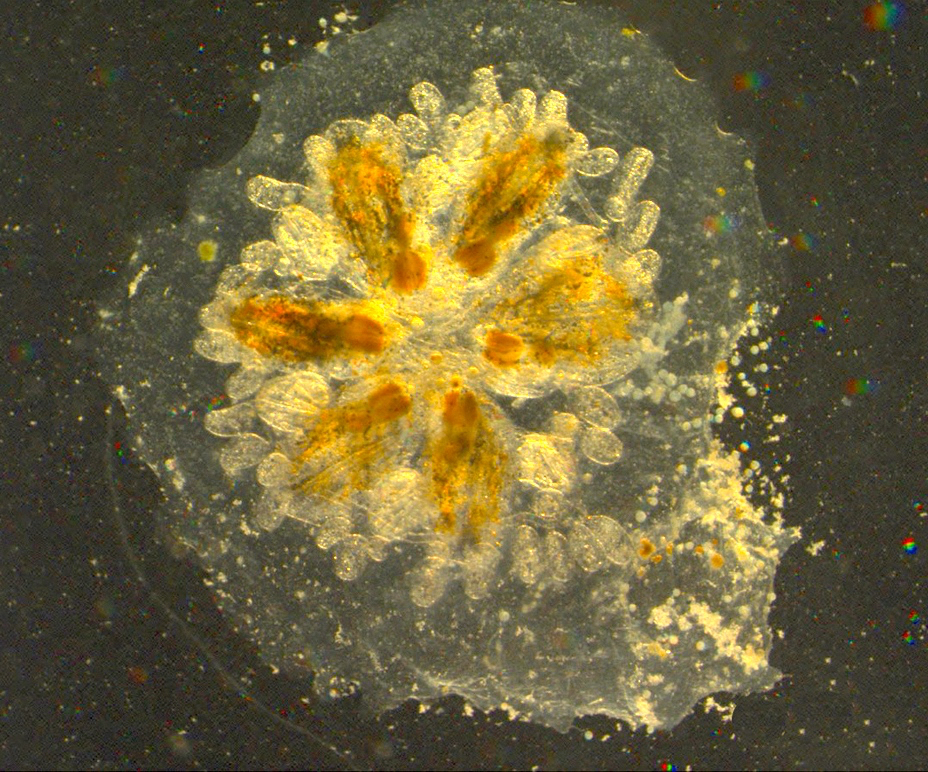
It’s a tiny marine invertebrate, no more than 3 millimeters in size. But closely related to humans, Botryllus schlosseri might hold the key to new treatments for cancer and a host of vascular diseases.
Using Botryllus — more commonly known as star ascidian — researchers at UC Santa Barbara have developed a new way to study the biology of blood vessels that may one day contribute to just such scientific discoveries.
Growing in colonies composed of many multicellular animals, the star ascidian has a massive, transparent vascular network located outside its collective body. This permits detailed study of vascular mechanics and by extension vascular disease — a malady that affects 1 billion people worldwide.
The scientists focused in particular on the interaction of cells and their physical environment, which includes changing the stiffness of a part of the blood vessels that reacts by withdrawing. Their findings appear in the journal Molecular Biology of the Cell.
“We can actually tune the stiffness, which is something that cannot be done in other model organisms,” explained corresponding author Anthony De Tomaso, an associate professor in UCSB’s Department of Molecular, Cellular, and Developmental Biology. “This has important implications, from inducing blood vessels to regress away from a tumor and choke off its oxygen and nutrients to the ability to stretch and hold an individual blood vessel and study how it responds, which will allow us to study how shape emerges during development.”
When the scientists excised a section of Botryllus vasculature and plated it on a surface coated with collagen, they found growth greatly improved. Collagen resembles the extracellular matrix (ECM) on which the star ascidian reproduces.
“This was surprising,” De Tomaso said. “How did this animal know it was on collagen and how did it know to respond differently?”
The answer began with lysyl oxidase, a protein that regulates the stiffness of the ECM. When the investigators added a lysyl oxidase inhibitor to the water in which the ascidians grew, it caused their blood vessels to regress. Somehow the inhibitor was telling the vasculature to withdraw and get smaller. But how?
De Tomaso’s team worked with Megan Valentine, an associate professor in the Department of Mechanical Engineering, whose lab studies how physical forces control cellular outcomes. Together, the scientists dug deeper to determine the mechanisms behind the regression. It turns out that proteins called integrins protrude from the cells and not only grab onto the ECM but also hold on to one another.
“There’s a mechanism in all epithelia — cells that maintain a barrier function like the skin or blood vessels — that allows this regression to occur,” De Tomaso explained. “We found that when we affected integrin’s ability to hold on, a subset of cells along the ECM began to die in some coordinated fashion that we don’t understand. The cells get squeezed out, are eaten by other cells in the blood, and that’s how the vessel shrinks — all without impeding the flow of blood through the vessels.”
The investigators then dissected different pathways, including a phenomenon called anoikis, which prevents epithelial cells from changing into other cell types by causing them to commit suicide. Anoikis is important because 90 percent of human cancers are carcinomas that originate in the epithelium. In order for metastasis to occur, cancer cells have to overcome anoikis.
“Understanding how a cell interacts with its physical environment has important implications for understanding both cellular development and metastasis,” said co-author Valentine. “Botryllus has given us the ability to dissect exactly what’s going on when we change the physical environment.”
The two UC Santa Barbara labs are continuing this work by performing a variety of physical manipulations they hope will illuminate how tissues sense and process mechanical signals in development and regeneration.
Additional contributors are lead authors Delany Rodriguez and Brian Braden and co-authors Scott Boyer, Daryl Taketa, Leah Setar, Chris Calhoun, Alessandro Di Maio and Adam Langenbacher.
This work was supported by the G. Harold and Leila Y. Mathers Foundation, the National Institutes of Health, the National Science Foundation and the Gordon and Betty Moore Foundation.